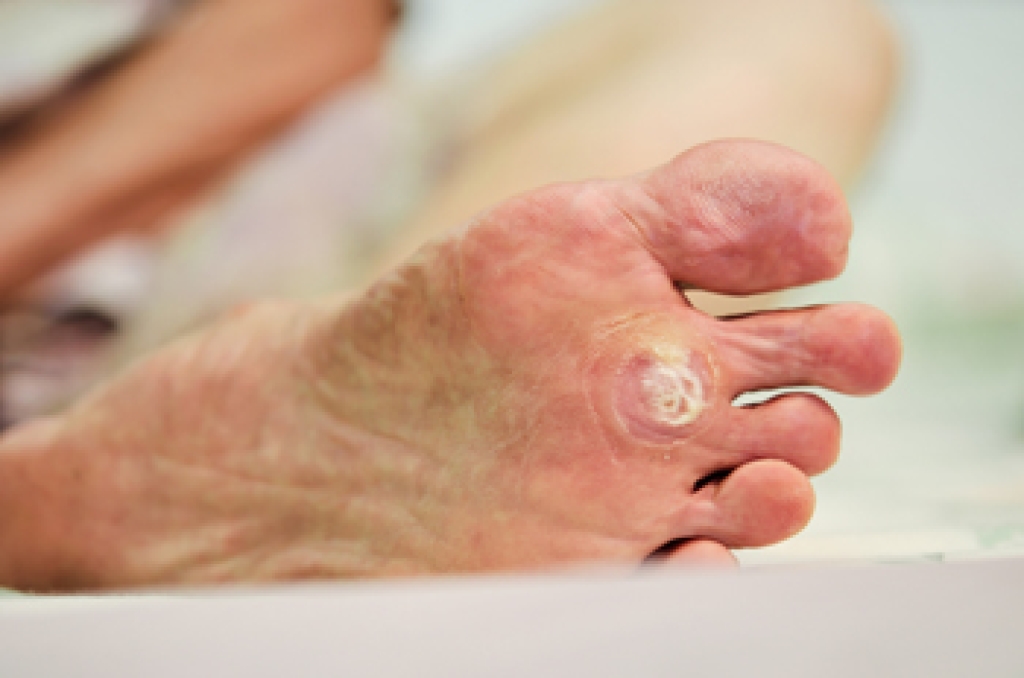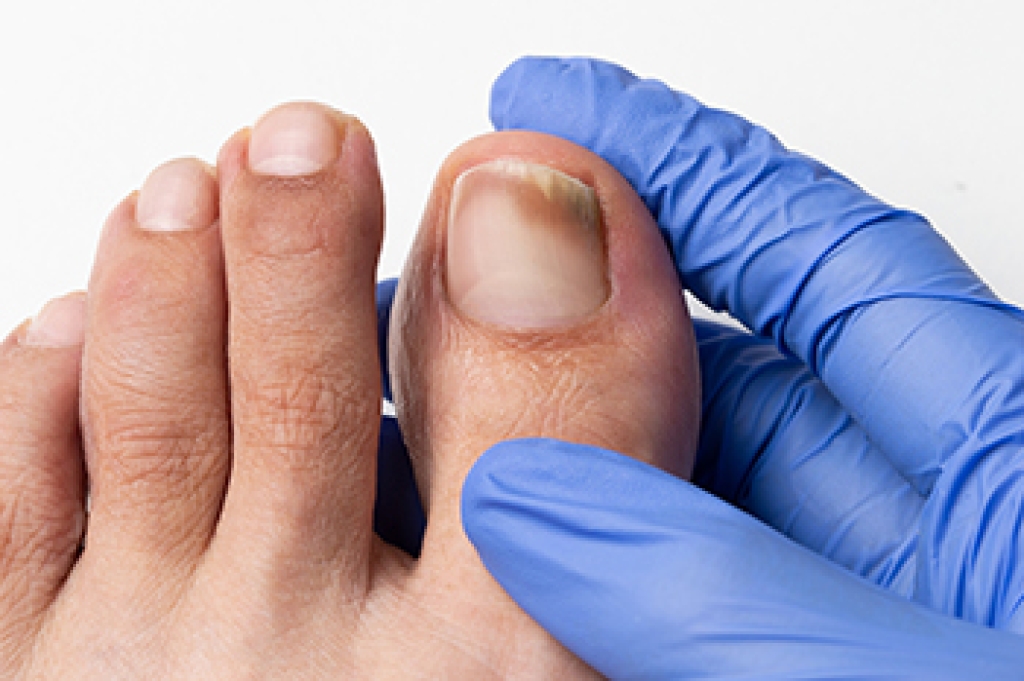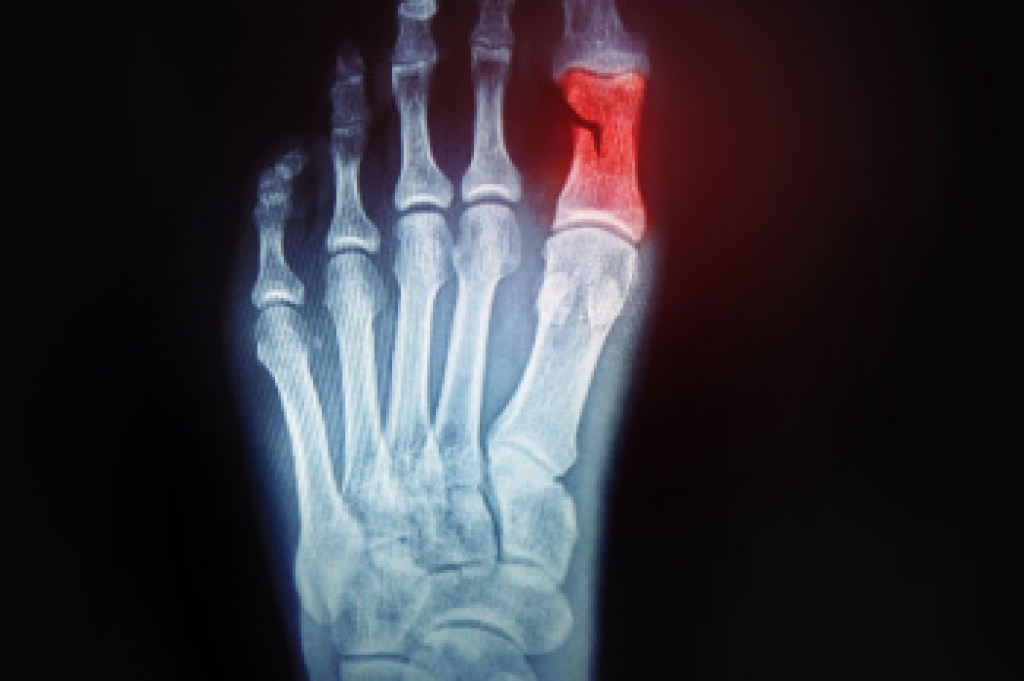
Pain in the ball of the foot, also known as metatarsalgia, is a common condition that can make standing, walking, and running uncomfortable. It occurs when the tissues surrounding the metatarsal bones become inflamed or irritated, often due to excessive pressure, overuse, or injury. Causes include high impact activities, wearing poorly fitted shoes, foot deformities, and obesity. Risk factors include high arched feet, bunions, hammertoes, and repetitive stress from sports or prolonged standing. Symptoms include sharp or burning pain, swelling, numbness, and difficulty bearing weight. A chiropodist can evaluate the underlying cause, provide orthotics, suggest proper footwear, and recommend therapies to reduce pain and restore function. If you are experiencing persistent discomfort in the ball of your foot, it is suggested that you consult a chiropodist today for the treatment that is right for you.
Foot pain is a common problem treated by chiropodists. If you have foot pain, please consult with one of the specialists from Thornhill Foot Clinic. Our chiropodists can help you maintain the health of your lower limbs and your mobility.
When you are experiencing foot pain, it’s important to note the type of pain and its location, as this can help determine a diagnosis.
Pain in the top of the foot may be caused by:
- Stress fractures
- Sinus tarsi syndrome
- Extensor tendonitis
- Tibialis anterior tendonitis
- Gout
- Athlete’s foot
- Ganglion cysts
Pain in the bottom of the foot may be caused by:
- Plantar fasciitis
- Foot cramps
- Tarsal tunnel syndrome
- Plantar fibromatosis
- Posterior tibial tendonitis
- Stress fractures
- Flat feet
Pain on the side of the foot may be caused by:
- Ankle sprain
- Cuboid syndrome
- Peroneal tendonitis
- Stress fractures
- Bunions
- Corns or calluses
- Posterior tibial tendonitis
Heel pain may be caused by:
- Plantar fasciitis
- Achilles tendonitis
- Bone spurs
- Heel fractures
- Retrocalcaneal bursitis
- Sever’s disease
Pain in the toes may be caused by:
- Gout
- Hammertoe
- Turf toe
- Bunions
- Ingrown toenails
- Blisters
- Arthritis
These and many more conditions can be treated by a chiropodist. If you have any questions please feel free to contact our office located in Vaughan, ON .