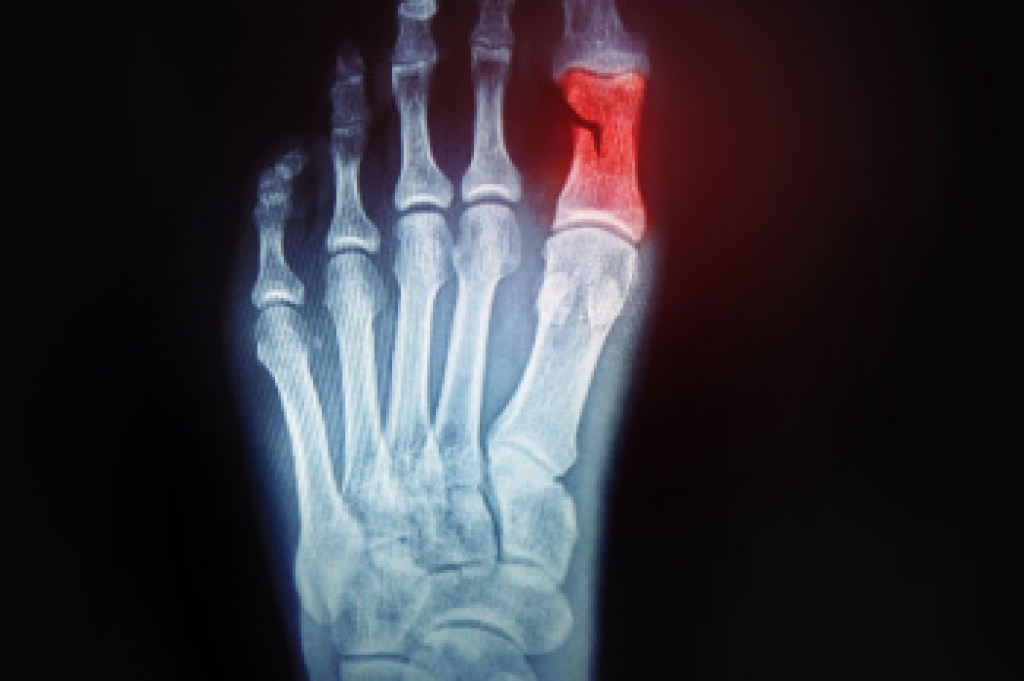
A broken toe occurs when one of the bones in the toe experiences a crack or complete break, often due to trauma such as stubbing the toe or dropping something heavy on the foot. This injury can cause immediate pain, swelling, bruising, and difficulty walking. Although some broken toes heal without surgery, proper care is essential to avoid long-term discomfort or complications. Relief begins with resting the foot and avoiding activities that add pressure. Elevating the foot can help reduce swelling, and wearing stiff-soled shoes may provide support during recovery. If you have fractured your toe, it is suggested that you promptly contact a chiropodist who can offer you appropriate treatment tips.
A broken toe typically occurs following either a sudden, traumatic injury, like dropping a heavy piece of furniture on the toe. The impact causes the bone to fracture and produces a variety of painful symptoms. If you suspect that you’ve broken your toe, please consult with one of the specialists from Thornhill Foot Clinic. Our chiropodists can help you maintain the health of your lower limbs and your mobility.
Symptoms
- Throbbing pain
- Swelling
- Bruising
- Cracking sound at the time of injury
- Difficulty bearing weight on the toe
- Difficulty walking
- Toe resting at an unnatural angle
Diagnosis
Your chiropodist can diagnose a broken toe through physical examination and imaging studies, such as X-rays.
Treatment
The main goals of treatment are to ensure that the bone heals properly, as a toe fracture that doesn’t heal properly can lead to osteoarthritis. You will typically need to rest the affected toe. You may be prescribed a splint to immobilize the toe while it heals. Icing the affected toe and taking over-the-counter medications can help reduce pain. In cases of severe fractures, surgery may be necessary to reset the broken bones and make sure that they heal correctly.
If you have any questions please feel free to contact our office located in Vaughan, ON .